Overwhelmed and underresourced, health-care providers in rural Washington are struggling to meet patient needs. Students in an Intensive Capstone class stepped in to help bridge this gap and explore potential solutions using AI and Large Language Models (LLMs).
The course was designed by Information School guest faculty member Frank Martinez, who comes from a rural community in Yakima Valley. His experiences with disparities in health care inspired him to structure his class around building resources for rural health-care providers.
INFO 492, an eight-credit course, is among the iSchool's new Intensive Capstone course offerings. Introduced in the 2023-24 academic year, the courses allow students to complete the Informatics Capstone requirement in one quarter, as opposed to the two-quarter structure of the regular Capstone.
With an accelerated timeline, INFO 492 students dived right into research, testing the hypothesis of whether AI and LLMs can increase the capacity of rural health-care providers.
The class of 12 students was divided into six teams, each tasked with selecting a rural county in Washington state along with a specific practice area. The teams then reached out to providers in their respective counties to better understand the health-care challenges within their chosen contexts.
“My hope is that students walked away from this course with empathy for rural health care,” said Martinez.
Informatics student Katherine Zhang chose to focus her Capstone on elderly care in Adams County. During her team’s initial research, she was shocked by the trends she came across.
“I didn’t realize the extent of the shortage of health care in rural areas,” said Zhang. “In Adams County specifically, there’s maybe two providers for 10,000 residents, which is very troubling.”
Another team of students, Andrew Chiang and Ximing Sun, uncovered similar disparities researching pediatric health care in Ferry County.
“A fourth of the population is below the federal poverty level; there’s high rates of people unemployed and uninsured,” said Chiang. “This class has really opened up our perspectives and allowed us to understand the disparities between rural and urban health care.”
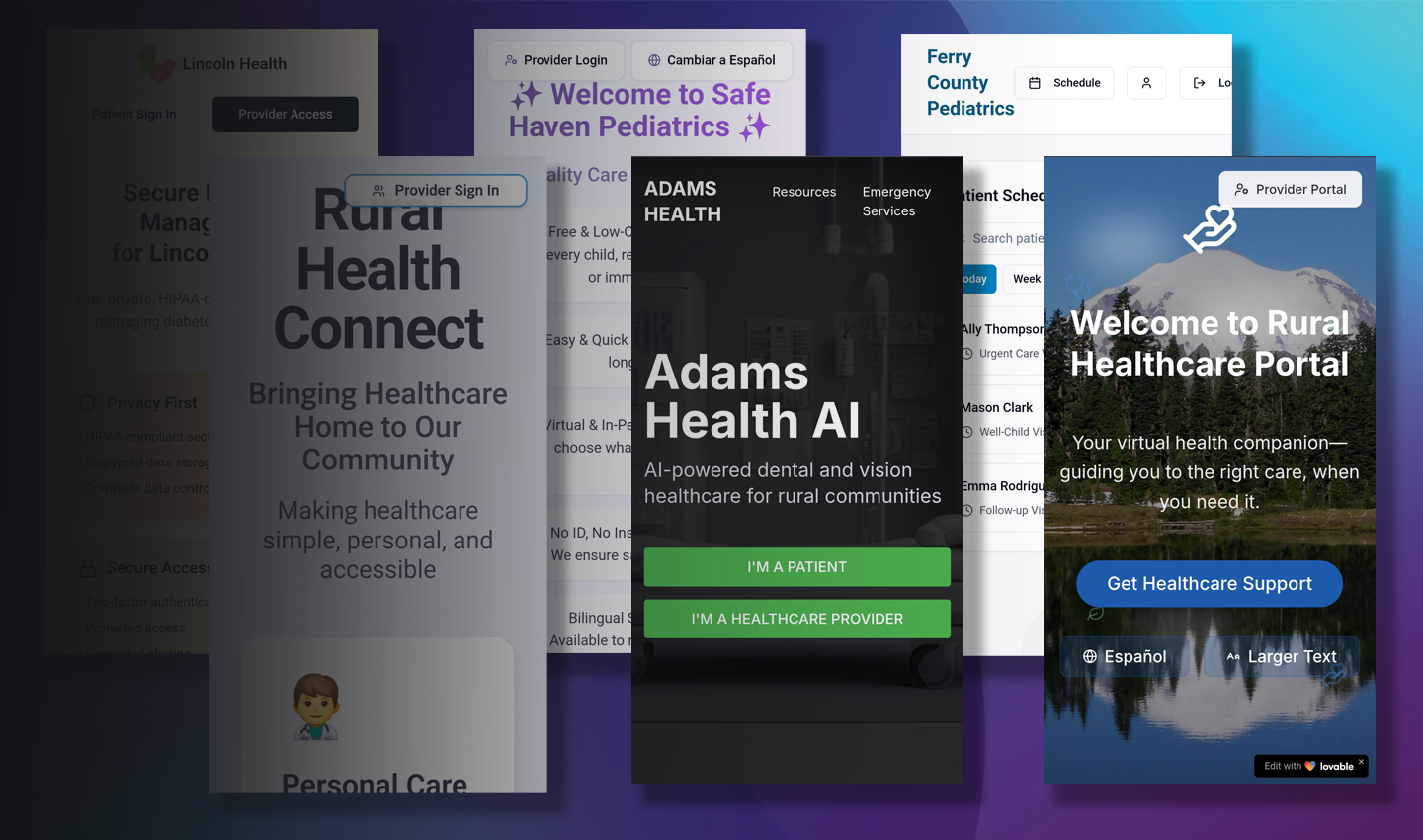
By the end of the quarter, the teams used their research to design and prototype virtual rural health-care clinics along with go-to-market presentations to outline what would be required to deploy the prototypes in practice. The virtual clinics involved creating synthetic personas of a rural patient and a health-care provider within their selected practice area. Students then leveraged LLMs for user testing, simulating interactions between the synthetic patient and provider.
“We definitely ran into some obstacles building the virtual clinics, but it was all an incredibly valuable experience because I feel like we came out of it more prepared to handle the rigor of working in the real world,” said Sun.
After 10 weeks of a challenging course load, students successfully produced six virtual clinic prototypes.
“Despite the intensity of this Capstone model, a passion for health care and commitment to underserved communities motivated everyone in this class and really empowered students to succeed,” said TA and Informatics student Vikram Murali.
“The prototypes students have created really show what’s possible with new technologies in rural health care,” said Martinez. “I hope this will open the door for more research and bring some much-needed attention to rural health care in Washington.”